4 Questions to Ask Before Back Surgery
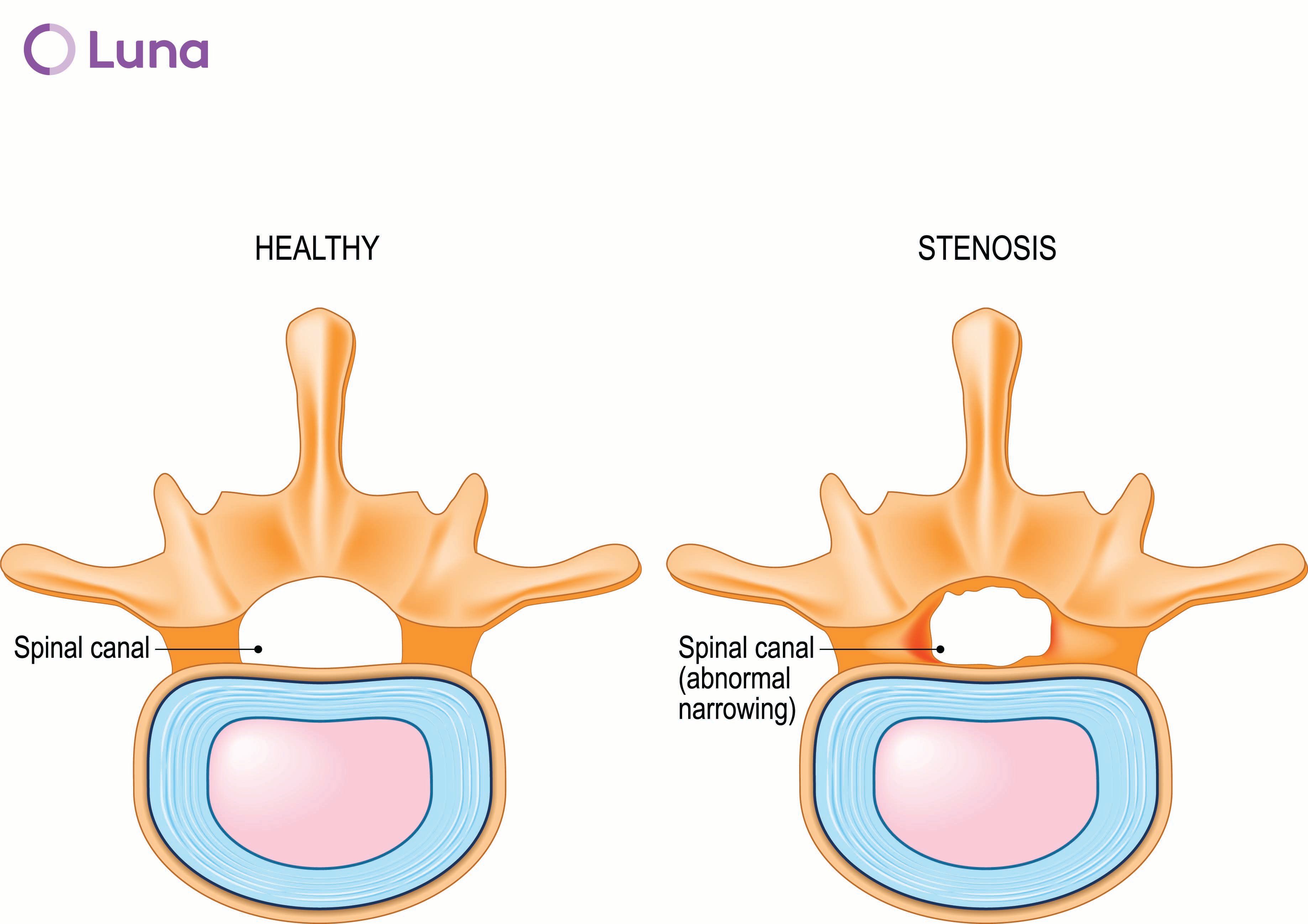
Ouch! Your lower back is in serious pain, and your left leg feels weak. Walking hurts. You’ve been diagnosed with spinal stenosis, a condition that occurs when the space around the nerve roots of the spine become compressed. Despite rest, a short course of steroids, and a few visits to the chiropractor, you’re just not feeling better, so your doctor recommends surgery.
You may feel unnerved by the concept of back surgery. There are risks, after all: reaction to anesthesia, bleeding, infection, a herniated disc, and nerve damage. Thanks to newer procedures, back surgery is safer than ever before.
“Treatments for spinal conditions have improved significantly in the last five to 10 years,” says Dr. Addison Stone, a spine surgeon near Seattle, Washington. “We are now able to make smaller incisions so patients have faster recoveries, less pain, and overall better outcomes.”
Questions to Ask Your Spine Surgeon: Insight from Dr. Addison Stone
What is minimally invasive spine surgery?
- Minimally invasive spine surgery represents a surgical philosophy to minimize soft tissue damage that normally occurs during surgery. This involves not only making smaller incisions but also limiting the amount of soft tissue disruption beneath the skin. While the incisions may be considerably smaller than standard incisions, the procedure performed is essentially the same.
- It significantly reduces post-operative pain and provides a much faster recovery. In addition, infection rates are significantly lower with minimally invasive techniques. Advances in surgical techniques, as well as equipment, allow surgeons to perform minimally invasive surgery for many procedures that were never thought possible.
- A patient and surgeon should be on the same page with respect to the goals of the surgery. For example, surgery for a pinched spinal nerve is often performed to treat symptoms down the arm or leg (pain, numbness, and/or weakness). If a patient’s main reason for having surgery is to treat neck or back pain, they may not be happy with the results.
- The surgeon will think surgery was a success if the patient’s arm or leg symptoms resolved, but the patient will not be satisfied since they will likely still have chronic neck or back pain. These types of situations can be avoided with proper communication between a surgeon and a patient prior to surgery.
- Most patients assume their surgeon will perform their surgery. However, surgeons in training often perform many of the procedures in teaching hospitals. This is good to know prior to surgery. This practice is safe as long as the “surgeons in training” are adequately supervised.
Physical Therapy and Your Spine
Physical therapy can be an effective treatment for spinal stenosis or other back problems. PT treatments involve a combination of manual therapy, postural education, and exercises. The goal of spinal stenosis PT is to reduce your discomfort and help you return to normal daily activities. Manual therapy and postural education can both help ease pain, and exercises improve mobility.
If your back pain makes a trip to the clinic difficult, consider on-demand physical therapy. You’ll receive expert, one-on-one time with a physical therapist who’s focused on one thing—helping you heal. Check out Luna’s on-demand physical therapy services in the Bay Area, Los Angeles, Orange County, and now Seattle!




